Telehealth for Mental Health: How virtual platforms are reshaping behavioral healthcare

62% of telehealth claims involve mental health. Explore how virtual platforms improve access to therapy, reduce no-shows, and support scalable behavioral health programs.
In February 2025, 62.3% of patients with a telehealth claim had a diagnosis related to mental health (Source: Grow Therapy, 2025). Mental health is no longer a secondary use case for telehealth, it is the primary driver of sustained virtual care adoption. The U.S. digital mental health market is projected to reach $8.97 billion in 2026, growing at a CAGR of 20.25% through 2035 (Source: Towards Healthcare, 2025).
This article examines why telehealth has become the default delivery channel for behavioral health services, what clinical conditions it treats most effectively, the essential features of a telepsychiatry platform, the 2026 regulatory landscape, and how healthcare organizations can build or integrate tele-mental health solutions at scale.
I. Why Mental Health Dominates Telehealth Utilization
Psychiatry leads all specialties in telehealth adoption, and by a wide margin. While fields like dermatology and ophthalmology struggle to translate their workflows to virtual settings, mental health consultations are inherently talk-based. Video and audio-only platforms are sufficient for most therapeutic modalities, including cognitive behavioral therapy (CBT), dialectical behavior therapy (DBT), and psychodynamic therapy.
The provider shortage amplifies this dynamic. Over 160 million Americans live in Mental Health Professional Shortage Areas, according to HRSA. Telehealth eliminates the geographic constraint entirely, allowing a licensed therapist in New York to treat a patient in rural Montana – provided licensing requirements are met.
Stigma also plays a role that is often underestimated. Walking into a psychiatrist’s office still carries social friction for many patients. Virtual platforms let people access therapy from home, reducing that barrier significantly. Combined with the convenience of no commute and flexible scheduling, it is unsurprising that mental health became the dominant telehealth category.
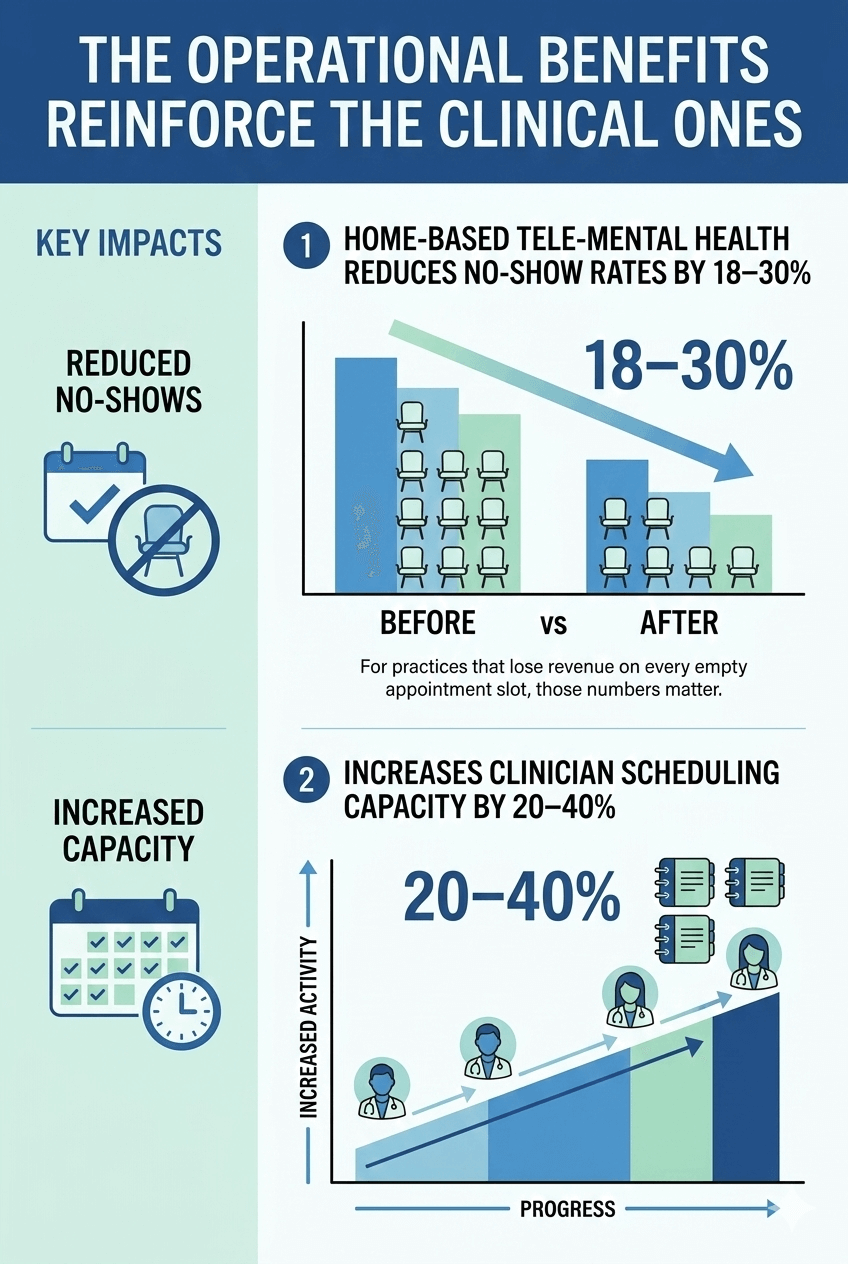
The operational benefits reinforce the clinical ones. Home-based tele-mental health reduces no-show rates by 18–30% and increases clinician scheduling capacity by 20–40%. For practices that lose revenue on every empty appointment slot, those numbers matter.
II. Clinical Conditions Best Suited for Telehealth Treatment
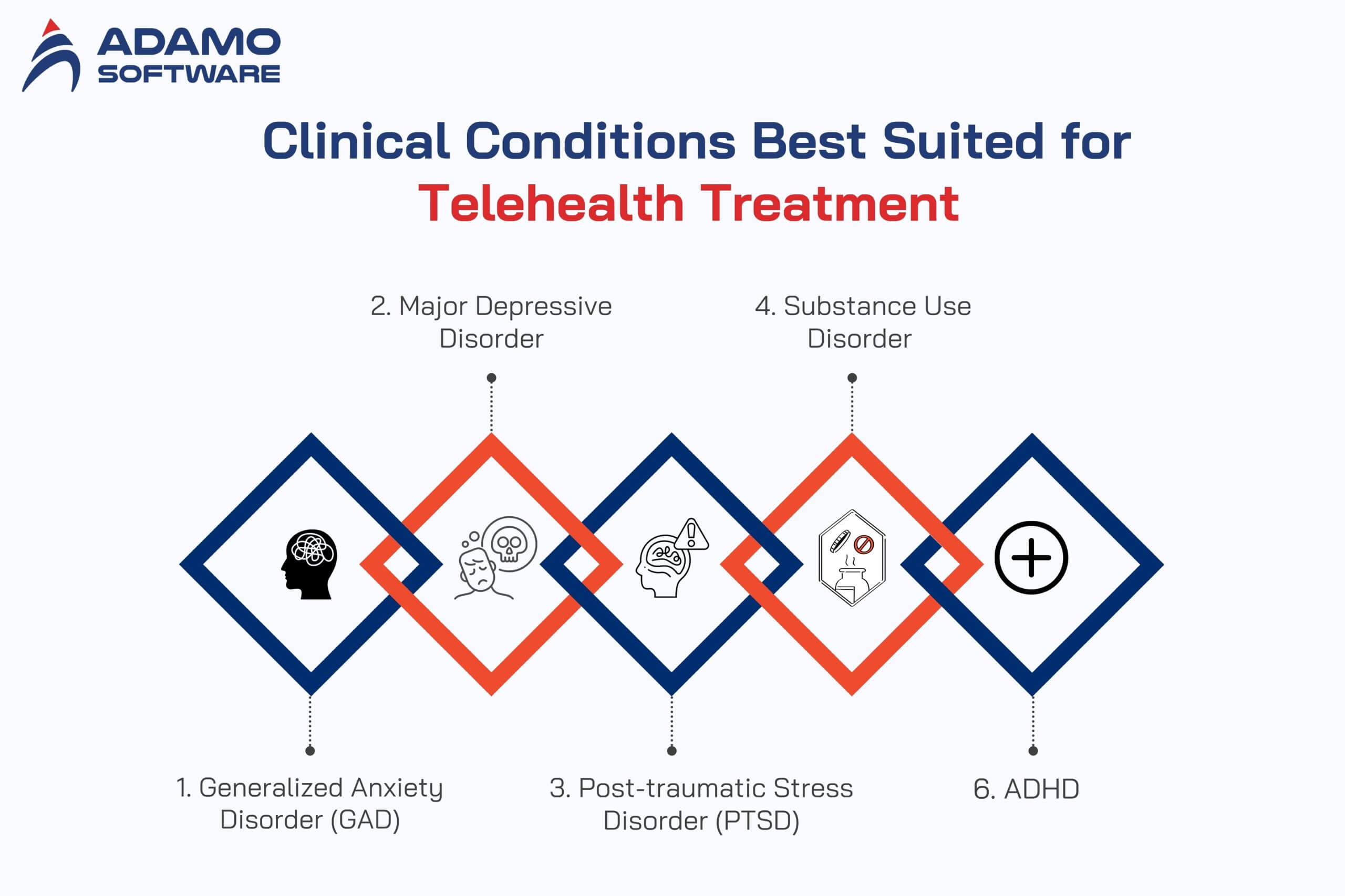
Not every mental health condition requires in-person care. Telehealth delivers equivalent clinical outcomes to face-to-face therapy for several common conditions:
- Generalized Anxiety Disorder (GAD): the most common telehealth mental health diagnosis. CBT delivered via video shows comparable symptom reduction to in-person sessions across multiple clinical studies.
- Major Depressive Disorder: medication management combined with virtual therapy sessions provides effective ongoing treatment. The ability to schedule frequent, short check-ins (15–20 minutes) is particularly valuable for medication titration.
- Post-Traumatic Stress Disorder (PTSD): trauma-focused CBT and EMDR have been adapted successfully for virtual delivery. Some patients actually report feeling safer discussing traumatic experiences from their own environment rather than an unfamiliar clinical setting.
- Substance Use Disorders: telehealth availability at substance use treatment facilities increased by 143% between 2020 and 2021. Physicians prescribing buprenorphine for opioid use disorder report that telehealth has meaningfully improved both access and treatment continuity.
- ADHD: virtual assessments combined with ongoing medication management have become a standard care pathway, particularly for adult ADHD patients who face scheduling barriers with traditional clinics.
Conditions requiring hands-on neuropsychological testing or inpatient stabilization remain better suited for in-person settings. However, telehealth serves effectively as a follow-up and maintenance channel even for complex cases.
III. Key Features of a Telehealth Platform for Mental Health
Building a telehealth solution specifically for behavioral health requires capabilities beyond standard video consultation tools:
- HIPAA-compliant video conferencing with end-to-end encryption, supporting both individual and group therapy sessions. Group therapy is increasingly reimbursed under the 2026 CMS Physician Fee Schedule, making this communication tool for telehealth a revenue-critical feature.
- Audio-only telehealth support. Medicare permanently allows audio-only delivery for behavioral health services. This matters more than most developers realize — many patients in rural areas or older demographics lack reliable video capability, and excluding them means excluding a large portion of the addressable market.
- Secure asynchronous messaging for between-session communication. Patients need a way to message their therapist with non-urgent concerns, medication questions, or crisis alerts without scheduling a full appointment.
- Integrated e-prescribing for controlled substances. The DEA extended telemedicine prescribing flexibilities for Schedule II-V medications through December 31, 2026. Platforms must support electronic prescriptions for SSRIs, SNRIs, stimulants, and buprenorphine.
- EHR integration providing therapists with real-time access to patient history, session notes, medication records, and treatment plans during virtual sessions. Without this, clinicians waste the first five minutes of every session catching up on context.
- AI-powered session documentation that transcribes and summarizes therapy sessions. This alone can save therapists 30–45 minutes of administrative work per day — time that translates directly into additional billable sessions.
- Patient self-assessment tools including PHQ-9 (depression), GAD-7 (anxiety), and PCL-5 (PTSD) screenings completed before each session. These give clinicians objective data to track treatment progress over time rather than relying solely on subjective patient reports.
- Automated scheduling and reminders via SMS and email. Combined with the low-friction nature of virtual visits, proper reminder systems can push no-show rates below 10%.
IV. Regulatory Landscape for Tele-Mental Health in 2026
The regulatory environment for tele-mental health has become more favorable than at any point in history, though complexity remains.
The 2026 CMS Physician Fee Schedule permanently established several critical protections. Geographic restrictions have been permanently removed for mental health services. Patients can receive behavioral health telehealth from their homes on a permanent basis. Audio-only telehealth for mental health is permanently allowed. Licensed psychologists, clinical social workers, counselors, and marriage/family therapists are all recognized as eligible distant-site providers.
Cross-state licensing remains the biggest operational headache. Over half of U.S. states still do not allow cross-state telehealth practice. Providers must hold active licenses in the state where the patient is physically located during the session. Compacts like PSYPACT (for psychologists) and the Interstate Medical Licensure Compact are expanding, but adoption is not universal. Any organization planning multi-state tele-mental health services needs a licensing strategy from day one – not as an afterthought.
For controlled substance prescribing, the DEA extended COVID-era flexibilities through December 31, 2026, allowing telemedicine prescriptions without an initial in-person visit. Whether these flexibilities become permanent or expire will significantly impact how tele-psychiatry platforms operate in 2027 and beyond.
Turn your ideas into scalable software
Adamo Software helps businesses design, build, and scale high-quality digital solutions with experienced engineering teams.
V. Building vs. Buying: Platform Strategy for Healthcare Organizations
Healthcare organizations considering tele-mental health face a classic build-versus-buy decision.
Adopting an existing platform like Teladoc, Amwell, Talkspace, or Cerebral offers faster time-to-market and lower upfront costs. These platforms handle compliance, infrastructure, and provider networks. The tradeoff: limited customization, restricted data ownership, and per-visit fees that erode margins as volume scales. For organizations testing tele-mental health as a new service line, starting with an existing platform makes sense.
Building a custom telehealth platform provides full control over features, data, branding, and integrations. Custom telemedicine app development solutions connect directly with existing EHR systems, billing workflows, and patient portals. The upfront investment is higher, but organizations retain ownership of patient data and can differentiate their service offering in competitive markets. For health systems planning to deliver thousands of sessions per month, custom development typically delivers better long-term ROI.
A hybrid approach: building a custom front-end on top of established telehealth APIs like Twilio, Vonage, or WebRTC – balances speed, cost, and customization. This is the path most mid-sized organizations find optimal.
VI. Conclusion
Telehealth is not a supplementary channel for mental health care – it is becoming the primary one. With permanent Medicare policy support, strong patient preference, and a market growing at over 20% annually, healthcare organizations without a tele-mental health strategy face both clinical and commercial risk. The technology and regulatory framework are aligned. The remaining challenge is execution: building secure, scalable, clinician-friendly platforms that deliver therapeutic outcomes equivalent to in-person care while operating profitably at scale.
VII. Build a Scalable Tele-Mental Health Platform With Adamo
Adamo Software helps behavioral health providers build secure telepsychiatry platforms: from HIPAA-compliant video consultations and integrated e-prescribing to AI-powered session documentation and EHR connectivity. Whether you are launching a new tele-mental health service or scaling an existing one, our team handles the technical complexity so you can focus on patient care.
Contact us for a free consultation: https://adamosoft.com/contact-us/





